Challenges, Implications, and Strategies for Accurate Diagnosis
The misdiagnosis of skin conditions is a persistent challenge in the field of dermatology, with implications that can significantly impact patients’ well-being. One particularly complex and often overlooked aspect of misdiagnosis involves the confusion between bed bug bites and other skin conditions. Bed bugs, once nearly eradicated, have made a resurgence in recent years, leading to an increased incidence of individuals seeking medical attention for skin issues that may be incorrectly attributed to other causes.
In this article, we delve into the nuances surrounding the misdiagnosis of bed bug bites by dermatologists, explore potential reasons behind these misdiagnoses, and offer strategies to enhance accurate diagnosis and effective treatment.
The Resurgence of Bed Bug Infestations and Skin Complaints
1.1 A Global Reemergence
Bed bugs, scientifically known as Cimex lectularius, have become a significant public health concern worldwide due to a combination of factors including increased international travel, pesticide resistance, and changes in pest management practices. This resurgence has led to an escalation in individuals reporting skin issues that they suspect are the result of bed bug bites.
1.2 Variable Reactions and Diagnostic Challenges
One of the main complexities in diagnosing bed bug bites lies in the wide variability of individual reactions. While some people exhibit immediate and pronounced skin responses, others may show delayed or even minimal symptoms. This variability makes it challenging for dermatologists to definitively attribute symptoms to bed bug bites, potentially leading to misdiagnosis.
The Complexities of Misdiagnosing Bed Bug Bites
2.1 Visual Similarities to Other Skin Conditions
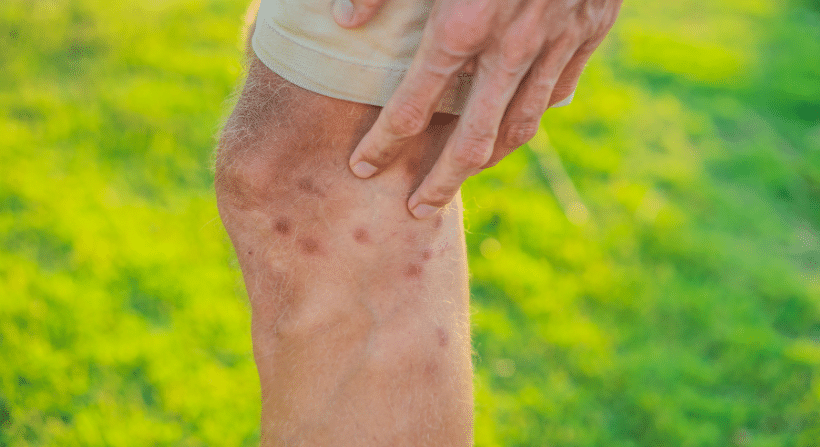
Bed bug bites often share visual characteristics with other common skin conditions such as hives, eczema, allergic reactions, and contact dermatitis. The similarity in appearance poses a significant hurdle for accurate diagnosis, as dermatologists may mistakenly identify these bites as another dermatological issue.
2.2 Lack of Training and Recognition
The resurgence of bed bugs and their associated bites is relatively recent. As a result, many dermatologists might not have been extensively trained in recognizing the distinctive features of bed bug bites. This lack of familiarity can lead to misdiagnosis, as dermatologists might not consider bed bug bites as a potential cause for skin complaints.
2.3 Diagnostic Bias and Assumptions
Clinicians may inadvertently bring biases and assumptions into their diagnostic process. The assumption that bed bug infestations only occur in unsanitary environments can lead to overlooking potential cases, as patients from all walks of life can experience infestations. Dermatologists need to approach each case with an open mind and without preconceived notions.
Section 3: Factors Contributing to Misdiagnosis
3.1 Patient Hesitation and Embarrassment
Patients experiencing skin issues that they believe are due to bed bug bites may hesitate to openly discuss the possibility of an infestation. The stigma and embarrassment associated with infestations can deter patients from seeking help and sharing critical information, leading to incomplete diagnostic evaluations.
3.2 Lack of Collaborative Approach
Dermatologists often work in isolation, but a collaborative approach involving pest management professionals can lead to more accurate diagnoses. Pest management experts can inspect living environments for signs of infestations and provide valuable information that aids dermatologists in their diagnostic decisions.
3.3 Inadequate Communication
Effective communication between patients and dermatologists is essential for accurate diagnosis. However, patients might not provide comprehensive medical histories, omitting information about potential exposure to bed bugs. Dermatologists should encourage open dialogue to ensure all relevant information is considered.
Strategies for Accurate Diagnosis and Treatment
4.1 Education and Training
To address the lack of familiarity among dermatologists, education and training on bed bug bites should be integrated into medical curricula. Workshops, seminars, and resources should emphasize the distinct features of bed bug bites and equip dermatologists with the knowledge needed for accurate diagnosis.
4.2 Diagnostic Guidelines and Algorithms
Developing clear diagnostic guidelines and algorithms for bed bug bites can aid dermatologists in their decision-making process. These guidelines should highlight the differentiating features of bed bug bites from other skin conditions, enabling more accurate assessments.
4.3 Patient Education and Empowerment
Educating patients about bed bug infestations and bites can empower them to share relevant information with dermatologists. Patients should be informed that bed bug infestations are not indicative of personal hygiene and that seeking medical help is a responsible step towards resolving the issue.
4.4 Enhanced Collaboration
Establishing communication channels between dermatologists and pest management professionals can lead to more comprehensive assessments. Collaboration ensures that both medical and environmental factors are considered in the diagnostic process, increasing the accuracy of assessments.
Read Also: Dealing with Bed Bugs and Bed Bug Bites
Conclusion
The misdiagnosis of bed bug bites by dermatologists poses challenges stemming from visual similarities, lack of familiarity, patient hesitation, and communication gaps. By acknowledging and addressing these complexities, dermatologists can enhance their diagnostic accuracy and provide appropriate treatment for patients. Empowering dermatologists with education, emphasizing collaboration, and fostering open communication can contribute to improved patient outcomes and the effective management of bed bug infestations. Challenges, Implications, and Strategies for Accurate Diagnosis
If you’re struggling with a bed bug infestation and need professional assistance, don’t hesitate to contact Tulsa Bed Bug Exterminator. Our experienced team offers expert solutions tailored to your needs, helping you reclaim your home from bed bugs. Schedule a consultation today and take the first step towards a bed bug-free home.

Recent Comments